Clostridium tetani was originally discovered via relatively primitive means in 1884 by a German physician by the name of Arthur Nicolaier. He then determined C. tetani to be the cause of tetanus by injecting test animals with garden soil known to contain the bacteria, which resulted in the characteristic fatal muscle spasms of tetanus. The Japanese bacteriologist Shibasaburo Kitasato advanced Nicolaier’s findings by preparing a complete/pure culture of the bacteria in 1889 and developed antitoxin for use against tetanospasmin in 1890. Following these developments, Edmond Nocard determined that the tetanospasmin antitoxin induced passive immunity and can be used for treatment as well as preventative vaccination against tetanus. The tetanospasmin vaccine is a toxoid, which is a substantially weakened version of the original toxin, which is used to induce passive immunity in humans, effectively preventing future infection. The vaccine is not permanent and requires subsequent inoculations in intervals, which are commonly known as vaccine boosters.
Infections of C. tetani left untreated or ineffectively treated result in the commonly fatal tetanus central nervous condition. The neurotoxin tetanospasmin released from the bacteria affects the nervous system by infiltrating the central nervous system via peripheral nerves. The toxin then attaches to inhibitory motor nerve locations, preventing the release of glycine and gamma-amino butyric acid, which are inhibitory neurotransmitters. The result is uncontrolled muscle spasms due to the absence of inhibitory chemicals. Early symptoms are muscle spasms of the skull, typically affecting the jaw muscles, resulting in a involuntarily closed mouth (lockjaw), and associated rigidity, followed by widespread, uncontrolled muscle contractions. Affected organisms die from lack of nourishment, due to the inability to keep the mouth open and perform mastication and deglutition.
Figure 5 is the artist Charles Bell's rendition of a classic case of untreated tetanus.
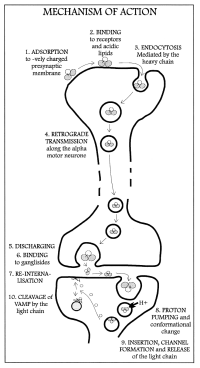
Figure 6 is a chart detailing the mechanism of a tetanospasmin molecule.